Always Catching Colds? Your Gut Might Be Part of the Story
If you’re getting frequent colds and lingering coughs, you might be wondering what’s going on with your immune system. While sleep, stress, and day-to-day load matter, gut health and the gut microbiome may also be part of the picture.
Do you seem to pick up every cold that’s going around, or feel stuck in a loop of coughs, sore throats, and lingering bugs? It’s easy to assume your immune system is simply “low”, and sometimes it is. Everyday life, young kids, a busy workplace, and little time to recharge can all take their toll.
A diet that is high in fibre can help support the microbiome
It’s also worth knowing that the gut microbiome may not be fixed. Its composition can shift over time, influenced by age and life stage, diet, stress, sleep, and environmental exposures, including antibiotics and wider chemical exposures. Collectively, these lifelong influences are sometimes described as the “exposome”. [1,2]
But there may be another piece of the jigsaw that’s often overlooked, your gut. Your digestive system, and specifically your gut microbiome, may be closely linked to immune function. Not in a direct “your gut causes colds” way, but in a more foundational way. When the gut is under strain, the immune system may find it harder to stay balanced and resilient. [1]
Why the gut may be linked to immunity
Your digestive tract is one of the body’s biggest contact points with the outside world. It’s sometimes described as being “outside” the body, because it’s essentially an open tube running from your mouth to your anus. Until nutrients cross the gut lining, what’s inside the digestive tract is still part of the external environment. [1]
In the context of infections, it can be helpful to think about gut defences as three overlapping layers, the resident gut microbiota, the gut lining, and the local immune system. Together, they reduce the chance that pathogens can take hold and cause problems. [1]
Factors influencing gut health
The gut lining is designed to be selective rather than “sealed off”. It’s a single layer of intestinal epithelial cells held together by tight junctions, which helps regulate what passes through and what stays out. [3]
At the same time, the large intestine, the colon, is home to the gut microbiome, a community of microorganisms including bacteria, viruses and fungi. In a healthy gut, this ecosystem supports digestion of fibre and helps maintain a stable environment, including colonisation resistance, where the existing microbiota helps reduce the ability of unwanted microbes to overgrow. [1]
This is one reason the gut is often described as a major immune hub. Some reviews estimate that around 70–80% of immune cells are present in the gut, reflecting how much immune monitoring and communication happens there day to day. [1]
The gut-lung link in simple terms
Because the gut is such an active immune ‘hub’, immune activity in the gut can influence immune activity elsewhere. One area of growing interest is the gut-lung axis, the idea that the gut and respiratory tract can communicate via immune signalling and microbe-derived compounds. [4]
When the gut environment is irritated or out of balance, the immune system may be working harder overall, which could influence how resilient the body feels during cold and flu season. This is not a direct cause-and-effect, but more a systems link that may help explain why digestion, inflammation, and “catching everything” can sometimes show up together. [1,4]
Respiratory infections, particularly viral infections, may also affect the gut microbiome and gut function during and after illness, which can add to that ‘run-down’ feeling, especially if sleep and appetite are off at the same time. [4]
There is some human evidence that gut-targeted approaches may also influence everyday respiratory infections. Research has found that certain probiotics may reduce the risk of acute upper respiratory tract infections, such as the common cold, although results vary by strain and population. [6]
What gut imbalance can feel like
What gut imbalance can feel like
A microbiome imbalance is often described as dysbiosis, essentially when the microbial community shifts away from its usual balance, for example, lower diversity, fewer supportive microbes, or a more reactive gut environment. [1]
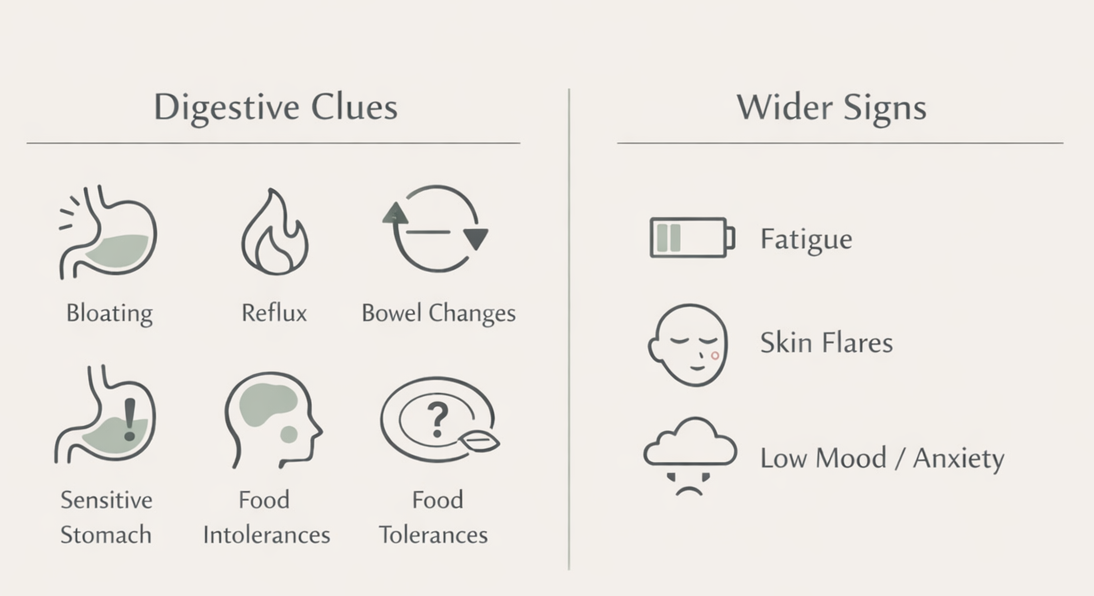
Common clues can include:
Bloating or excessive wind, especially after meals
Reflux, indigestion
Constipation, looser stools, or alternating between the two
Discomfort, or a “sensitive” stomach that feels unpredictable
Food tolerance narrowing over time
Some people also notice wider signs that can travel with gut strain:
fatigue, or feeling easily run down
skin flares that feel more frequent
low mood, or anxiety that seems worse when digestion is off
None of these symptoms prove dysbiosis on their own. They can have many causes. If they are recurring or clustering together, it may be a sign the gut environment would benefit from a steadier baseline. [1]
Why gut imbalance can happen so easily
The gut microbiome is responsive, which means it can be pushed off balance by ordinary pressures, especially when several happen at once, such as repeated infections (and sometimes antibiotics), higher stress and poor sleep, rushed eating and irregular meals, low fibre or low variety, alcohol when the gut is already irritated, and a stretch of convenience foods. [1,2]
High-fibre breakfast: oat & chia pudding with berries
Supporting gut health
Gut support does not need a complicated protocol. A simple “baseline” to come back to:
Fibre, slowly and with variety: build gradually, focus on variety across the week. Different fibres can influence the gut microbiota and short-chain fatty acid patterns, although responses vary from person to person. [5]. Replace white refined carbs with whole grains (brown rice, sourdough, quinoa, spelt).*
Eat more colourful veggies and fruit - lots of variety. Fruits like pears and kiwis contain lots of fibre and can help with constipation.
Regular meals: a calmer rhythm, fewer rushed meals, and lighter dinners in the evening, especially if reflux or bloating is an issue.
Gentle movement: a short walk after meals can support gut motility.
Sleep: treat sleep as an immune foundation for a few weeks if infections are frequent. Try the 3–2–1 rule:
3 hours before bed - finish eating
2 hours before bed - stop working
1 hour before bed - put screens away
And try to keep your sleep and wake times consistent.
Ease off on gut irritants: if the gut is flaring, consider a short window with less alcohol and fewer rich foods later in the evening.
Come back to foundations
Food
Movement
Sleep
Stress
These can shape your gut day to day - and a steadier gut may mean a steadier immune system.
*Increase fibre gradually rather than overhauling your diet overnight. Start by adding one extra fibre-rich food per day - such as swapping to whole grains or adding an extra portion of vegetables - and keep it consistent for a week before building further. If your gut is sensitive, prioritise cooked foods and increase fluids alongside fibre to help minimise bloating while your system adjusts.
Other nutrients & foods that support gut + immune health
Fermented foods
Live yoghurt, kefir, sauerkraut, kimchi - may help support microbial diversity.
Vitamin D
Important for immune regulation, particularly in the UK, where levels are often low.
Vitamin C–rich foods
Citrus, berries, peppers, broccoli - support normal immune function.
Zinc-containing foods
Seafood, meat, seeds, nuts - involved in immune cell function.
Protein
Needed to build immune cells and maintain the gut lining.
If you’re repeatedly catching colds or struggling with lingering coughs, it may be a sign that the body is under strain, and gut health could be one part of the wider resilience picture. [2] Supporting the gut is not a guarantee you won’t pick up bugs, but it may help you feel more robust overall, with steadier digestion, more consistent energy, and a system that feels less reactive.
***If you’re experiencing recurrent or unusually severe infections, persistent fevers, unexplained weight loss, night sweats, shortness of breath, or you’re concerned about your immune health, it’s important to speak with your GP. Also seek medical advice if you notice red-flag gut symptoms such as blood in your stool, persistent vomiting, a significant change in bowel habit that does not settle, severe abdominal pain, or symptoms that are steadily worsening.
References
Wiertsema SP, van Bergenhenegouwen J, Garssen J, Knippels LMJ. The interplay between the gut microbiome and the immune system in the context of infectious diseases throughout life and the role of nutrition in optimising treatment strategies. Microorganisms. 2021;9(2):452.
Merra G, Gualtieri P, La Placa G, Frank G, Della Morte D, De Lorenzo A, Di Renzo L. The relationship between exposome and microbiome. Microorganisms. 2024;12(7):1386. doi:10.3390/microorganisms12071386. PMID: 39065154.
Turner JR. Intestinal mucosal barrier function in health and disease. Nat Rev Immunol. 2009;9(11):799–809. PMID: 19855405.
Liu J, Hong W, Sun Z, Zhang S, Xue C, Dong N. The gut–lung axis: effects and mechanisms of gut microbiota on pulmonary diseases. Front Immunol. 2025;16:1693964.
Vinelli V, Biscotti L, Martini D, et al. Effects of dietary fibers on short-chain fatty acids and gut microbiota composition in healthy adults: a systematic review of randomized controlled trials. Nutrients. 2022;14(13):2559. doi:10.3390/nu14132559. PMID: 35807739.
Zhao Y, et al. Probiotics for preventing acute upper respiratory tract infections. Cochrane Database Syst Rev. 2022;8:CD006895. doi:10.1002/14651858.CD006895.pub4.